Top Surgery
Overview
Top surgery is a step in the transitioning process that can be incredibly meaningful. FTM, MTF, and non binary chest reconstruction, or top surgery as it is commonly referred to, can greatly reduce feelings of gender dysphoria, which can in turn reduce depression, anxiety, and self-consciousness. If you’re interested in undergoing top surgery, consider a visit to the Kryger Institute of Plastic Surgery.
Before & After Photos
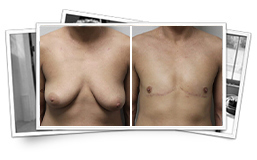 Top Surgery
Top Surgery
At the Kryger Institute of Plastic Surgery, we have experience in a vast array of surgical and non-surgical procedures. Click below to see some before and after photos of top surgery.
Ideal Candidates for Top Surgery
If you have experienced persistent and documented gender dysphoria, you are an ideal candidate for top surgery. Candidates must be age 18 or older, and a letter of support from a mental health professional will be necessary. Having undergone hormone treatments for at least one year is recommended. The best candidates for top surgery have already transitioned socially. If you are under the age of 18, surgery will be considered on a case by case basis.
Non-smokers are excellent candidates for top surgery. If you are a smoker, you will need to avoid smoking for several weeks before the date of your surgery. This is necessary because smoking negatively affects the health of the tissues, resulting in an increased chance of complications during and after surgery. Obesity is also a risk factor for complications after surgery. Ideal candidates should have a body mass index (BMI) below 35, with a BMI of 40 being the maximum.
The Consultation
The top surgery process begins with a personal consultation with Drs. Kryger and their staff. This consultation gives patients the opportunity to communicate their needs and goals for their surgical procedure. Dr. Kryger will ask questions as needed to ensure full understanding.
Next, Dr. Kryger will perform a physical examination. He will go over the patient’s complete medical history, including allergies, pre-existing conditions, past procedures, and current medications and supplements. Please make sure to tell us about all medications you use, including self-prescribed substances.
Dr. Kryger will then create a detailed surgical plan for the patient. He will explain the procedure in depth, starting with preparation directions and going all the way through the recovery process. Questions are highly encouraged and can be asked at any time.
Patients will then meet with the surgical coordinators who will discuss the insurance process. After we receive authorization from insurance, a date will then be scheduled for the patient’s top surgery.
Patients from out of town or who live a long distance from Thousand Oaks, CA. can do a virtual consultation.
Does insurance cover Top Surgery?
Most insurance companies cover top surgery, however this is done on a case by case basis. The Kryger Institute will do everything possible to work with your insurance carrier to obtain approval for your procedure. If the insurance company denies coverage for your surgery, we will try and appeal it. If we are unsuccessful, the cost of surgery will be your responsibility. Make sure to speak to our patient care coordinator about these issues ahead of time.
MTF Top Surgery
MTF, or male-to-female, top surgery involves surgical procedures to feminize the breasts. This includes various procedures such as the placement of breast implants in the chest, breast lift (mastopexy), and fat injections into the chest to create a small breast. This change can make a major difference in the transition process for transgender women.
Dr. Kryger will work with you to choose the ideal implants for your goals. There are numerous breast implant types, sizes, shapes, and profiles available, and the characteristics of your implants will greatly affect your results.
FTM Top Surgery
FTM, or female-to-male, top surgery removes the breasts, creating a more traditionally masculine chest for transgender men. This includes various procedures such as the double-incision mastectomy, periareolar, or keyhole mastectomies, and other techniques of chest masculinization.
Non Binary Top Surgery
For non binary patients, we offer a variety of procedures such as mastectomies, radical breast reductions, and nipple-free procedures for those patients who desire not to have nipples. During your consultation, Dr. Kryger will discuss your personal goals and desires and explain which procedure is best suited for you.
Body Masculinization or Feminization
At the Kryger Institute, we also offer a variety of surgical procedures to help create a more masculine or feminine body appearance. If this is something you are interested in, you should discuss this with Dr. Kryger and his staff. Some procedures can be done at the same time as the top surgery.
Revision of Previous Top Surgery
Drs. Kryger are experts in top surgery and have extensive experience in revising or correcting botched are less than ideal results. Many examples of corrective procedures can be seen in the office during your consultation.
Preparing for surgery
You will receive detailed instructions before surgery from your coordinator. You will need to pick up your prescription medications ahead of time. If you have chronic skin irritation below the folds of your breasts, bring this to the attention of Dr. Kryger so we can prescribe the appropriate treatment. Make sure to shower and wash the chest with antibacterial soap the night before surgery. If you have chest hair you should shave it a few days before surgery. You will be told which medications to stop and which to take before surgery. Aspirin and other blood thinners must be stopped for 7 days before surgery. Most diet medications such as Phenteramine, Ozempic and the like must be stopped a week before surgery. If you smoke, you must quit smoking entirely for 6 weeks before and 6 weeks after surgery. You must strictly follow the instructions about when to start fasting before surgery (usually at midnight). If you get sick or have any health issues in the days before surgery, please notify the office at once in case we have to postpone your operation.
The anesthesia
Top surgery is usually performed under general anesthesia. Occasionally, it can be performed under “twilight” anesthesia or local anesthesia for revision. Twilight anesthesia consists of intravenous sedation and pain medication that keeps you relaxed and sleepy during the surgery. In addition, the surgeon uses local anesthesia to numb the area. General anesthesia involves going completely to sleep with a breathing tube in your throat. There is a slightly higher risk of nausea and vomiting after general anesthesia, however both techniques are extremely safe. Your surgeon will discuss the anesthetic options with you before surgery.
Are drains used?
Top surgery does not routinely require the use of drains. It is a case by case decision and at the time of your consultation, Dr. Kryger will be able to inform you if he needs to use drains. Very large reductions or breast removal (especially if combined with liposuction) may require drains. This will be determined by your surgeon at the time of surgery. These drains help drain the fluid that is produced under your skin as part of the healing process. Without drains, this fluid can accumulate, termed a seroma. Drains stay in until the drainage is less than 25 ml per drain in a twenty four hour period. This usually takes several days, but can be shorter or longer in some cases. The drains are easy to take care of, and do not hurt to take out.
Can you go home the day of surgery?
Top surgery is always performed as an outpatient, and all patients will be able to go home the same day. This is safe and standard of care.
How much pain is there after surgery?
Pain from surgery is highly variable, and ranges from minimal to moderate. It is worst in the first few days after surgery, but then it rapidly improves. It is impossible to predict a person’s expected pain. If you have done well with surgery in the past, you will likely be fine after this surgery. Our surgeons have a lot of experience treating pain, and have published scientific articles and written book chapters about anesthetics and pain control. They will do everything possible to minimize your pain, including using pain pumps after surgery and utilizing all the newest pain medication. By the end of the first week, most people’s pain is controlled with plain Tylenol or Motrin.
What about swelling and bruising?
Swelling and bruising are normal signs of the healing process. They occur after any surgery to varying degrees. Swelling peaks at about 48 hours, and then rapidly decreases. By the end of the first few weeks, 50 percent of the swelling is gone. During this early period, your breasts will appear larger than their final size due to the swelling. By 6-8 weeks, a majority of the swelling has diminished. By six months, all the swelling is gone. Bruising is worst the day after surgery and then rapidly gets better. It is usually gone by two weeks. You may also experience a burning sensation in your nipples for up to two weeks, but this will subside as bruising fades.
What restrictions are there?
You can shower as soon as your surgeon gives you permission to do so. This ranges from one to five days, depending on the procedure. However, you should not submerge in a bath, use a hot-tub, or go swimming for at least two weeks. The first two days after surgery are usually spent doing minimal activity. Most patients then begin to get back to their regular routine. Within 3-5 days, you will probably be ready to leave the house for short trips and light walks. More vigorous walking and mild stretching exercises can be resumed about a week after surgery. Strenuous activities such jogging, aerobics, weight-training not be done until 6 weeks after surgery. Also, you shouldn’t do any heavy lifting (over 10 pounds) during this period. A good guide before beginning activities that involve direct contact to chest is to wait until pain and sensitivity in the chest or breasts has resolved.
When can I travel?
Traveling after surgery (air travel, long distance car trips, train rides, etc) should not be done before you have had your first postoperative visit. Typically, this occurs 5-10 days after surgery. Patients who are at high risk for developing a blood clot should not travel until instructed by their surgeon. Short car trips under 60 minutes can be done before the first visit. A good rule of thumb is when you are off the stronger pain medication and can get up without assistance you are ready to go for a short drive. You should not drive the car yourself, however, until your surgeon gives you clearance for this.
When can I go back to work?
This, of course, depends on the kind of work you do. Most people go back to work after one week. Sedentary jobs, such as computer work or talking on the phone can begin even sooner. If you have a strenuous job that involves a lot of lifting or physical activity, you may have to wait 3-4 weeks until you are ready for work. Please review the restrictions for further guidelines about getting back to work.
What kind of scars can I expect?
Scarring is an unpredictable part of any surgery. It is impossible to cut through the full thickness of the skin and not have a scar. For most patients, the incisions top surgery heal well and do not become bothersome scars. Our surgeons have published numerous scientific papers about the scarring process and wound healing, and will do everything possible to minimize scarring. To a large extent, however, scarring is determined by your genetics. If you are prone to hypertrophic (wide, raised) scars or keloids, make sure to inform your surgeon ahead of time. Our surgeons will use all the available techniques to minimize your scars based on their extensive research experience on hypertrophic scarring.
Your scars will be firm and pink for at least six weeks. After six weeks, scars are very strong and can withstand any activity. Then they may remain the same size for several months, or even appear to widen. After several months, your scars will begin to fade, although they will never disappear completely. It takes 1-2 years for a scar to completely heal. Make sure to apply sunscreen containing zinc-oxide to your scars for six months so that they do not darken due to increased pigmentation.

